Dry mouth or Xerostomia may be related to physiological conditions or environmental conditions. The physiological conditions include dental, and jaw malocclusions that lead to mouth opening, thus, dry mouth. The environmental and acquired conditions such as activity and mobility in extreme heat and failure to drink enough water also are causes of Xerostomia.
Dry mouth may result from some health problems including: diabetes, stroke, oral yeast infection (oral thrush), Alzheimer’s disease, or autoimmune diseases including Sjogren’s syndrome and HIV/AIDS. Snoring and open mouth breathing are also causes of xerostomia.
If there is absolutely no saliva, the patient cannot consume a simple biscuit without having to drink an immense amount of fluids. Moreover, we cannot taste the foods well. This is because many foods have to be dissolved in saliva so that the taste buds can receive and understand them. In the absence of saliva, teeth regularly wear out the tongue and cheeks and cause painful sores in the oral cavity. In the absence of saliva, we cannot speak easily because we may repeatedly cough, our lips stick to the surface of our teeth, and a thick foam embarrassingly accumulates around the corners of our mouth.
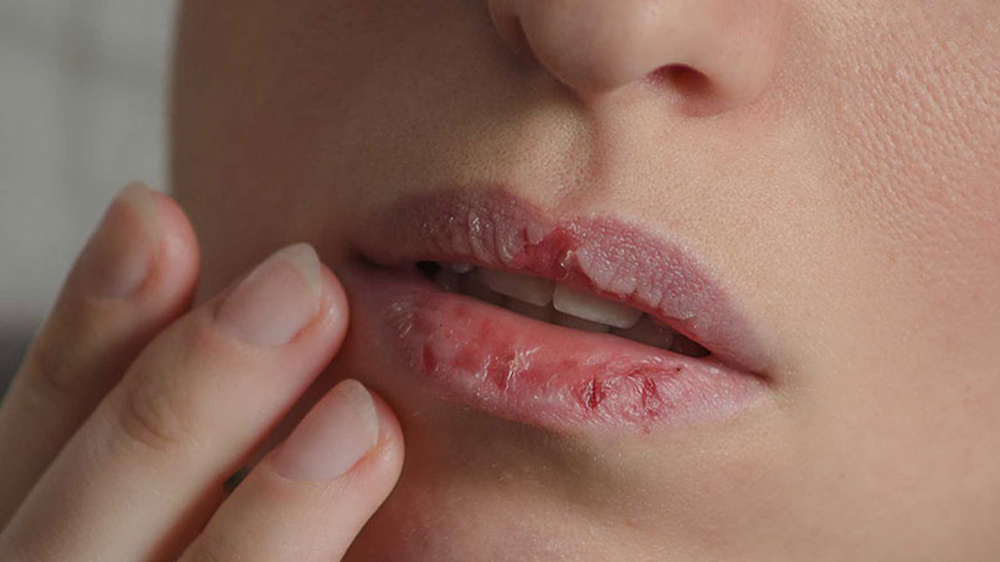
Xerostomia caused by the physiological conditions of the patient
The two rows of upper and lower teeth do not connect all the way in some patients with open bite malocclusion. These patients breathe with a half-open mouth and, if they do not visit an orthodontic specialist in time, will develop xerostomia or the other complications of this occlusion. Other dental and jaw malocclusions including overjet, short maxillary length, and Class 2 and 3 malocclusions may cause dry mouth. This is because patients suffering from them cannot always breathe through the nose and unconsciously breathe with their mouth open, which will lead to dry mouth and maxillary stenosis.
Neural, physical injuries in the head and neck area may cause Xerostomia. Saliva secretion also decreases with age. Thus, the patient must also drink more liquids, and water to compensate for it.
Xerostomia caused by environmental factors
Dry mouth caused by environmental factors can be controlled and treated by eliminating the environmental factors some of which are as follows:
- Tobacco and nicotine consumption
- Excessive alcohol, caffeine, tea and coffee consumption
- Radiotherapy and chemotherapy
- Consumption of neuropathic pain medications
- Poisoning
- Failure to drink sufficient water and liquids
- Work and activities in warm air
- Dental and oral infections
- Tooth decay
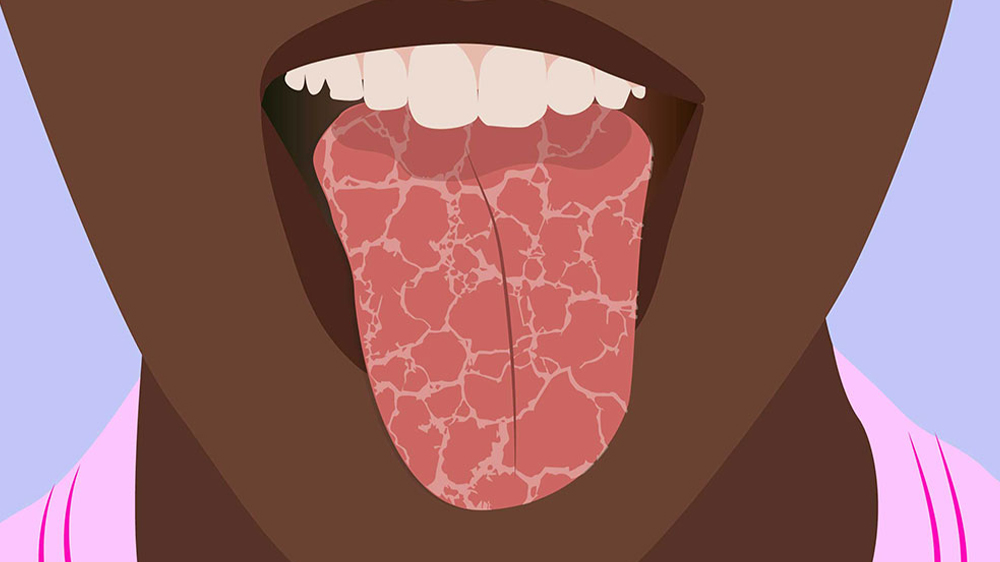
Treatment of dry mouth
Most dentists don’t take dry mouth seriously, and advise patients to drink more fluids. However, in some cases, that tip is useless. For example: What if the dry mouth is caused by Sjogren’s syndrome? Such cases of dry mouth won’t improve only by drinking more fluids. Most patients with Sjogren’s syndrome gradually become isolated because of their impaired speech. Some may feel that their tongue has enlarged and adversely affected their pronunciation. In a study conducted by Segal et al. in 2009, it was shown that patients with Sjogren’s syndrome pay for dental care three times more than normal individuals.
Dry mouth in patients with Sjogren’s syndrome may also pose problems for the dentist, exactly like recurrent dental caries along with very beautiful recent restorations. If such individuals have teeth filled with glass ionomer requiring regular local fluoride therapy, the restoration’s margin may break down, increasing the risk of tooth decay recurrence. When the patient has extensive cervical caries extended to the distal of the second molar, the story will be more complicated. This is due as, now, the dentist needs to shave and restore them!!

Home treatments for dry mouth
There was no standard protocol for dental treatment of dry mouth until 2016 when the Sjogren’s Syndrome Foundation (SSF) proposed guidelines to help prevent dental caries in patients with Sjogren’s syndrome. Local fluoride therapy may help prevent dental caries; however, this shouldn’t cause damage to glass ionomer fillings. Another way to prevent dry mouth is to stimulate salivation, by either increasing the chewing activity or taking drugs. The former is done by chewing sugar-free gums and the latter involves taking drugs such as pilocarpine Hydrochloride (Salagen) and cevimeline (Evoxac). Individuals who have extensive dental caries are recommended to use fluoride varnish, fluoride gels, or chlorhexidine mouthwashes to improve their dry mouth.
The most common & possibly the first symptom of Sjogren’s syndrome is dry mouth. It’s associated with extensive tooth decay. If a person with dry mouth is suffering from dry eye, articular pains, and fatigue, they are most likely afflicted with Sjogren’s syndrome, and need to visit an oral medicine doctor or a rheumatologist. In this disease, general dentists can play a major role in the timely diagnosis.

Causes of dry mouth FAQ
1-Is dry mouth dangerous?
Dry mouth is not dangerous by itself. It is often the symptom of a disease or abnormal condition in the body that requires examination and treatment. If the causal agent of dry mouth is not removed, it can lead to early tooth decay.
2-What are the complications of untreated dry mouth?
Saliva is a constituent of the body’s first line of defense. Dry mouth increases the risk of viral diseases such as influenza, and corona. Tooth decay and headache are among the serious long-term complications of dry mouth.
3-Is dry mouth a symptom of diabetes?
One of the most common symptoms of diabetes is dry mouth (xerostomia). It is a common symptom of type 1 and 2 diabetes; however, it’s important to note that not all diabetic patients experience it.
4-What are the diseases that cause dry mouth?
Diabetes, thyroid diseases, stroke, oral yeast infection (oral thrush), or Alzheimer’s disease are some of the diseases that cause dry mouth. Autoimmune diseases including Sjogren’s syndrome and HIV/AIDS may lead to xerostomia. Snoring and open mouth breathing, excessive consumption of tobacco, and alcohol also cause dry mouth.
5-Why do diabetic patients develop xerostomia?
Diabetic patients are susceptible to dry mouth and yeast infections such as thrush because of their high blood and salivary glucose levels. Low water content in the body of diabetic patients, smoking, and consumption of some medications are among the other reasons.






